
LEARNING OUTCOMES
By the end of this lecture students should be able to:
Explain how structural and intermediary factors interact to influence health outcomes using the Social Determinants of Health framework.
Describe the mechanism by which the social determinants of health contribute to differences in health outcomes within and between populations.
Apply the concepts of structural violence, structure and agency, implicit bias, and social exclusion to explain the influence on health inequities.
Analyze how the ecological model informs clinical and public health decision-making, recognizing the multi-level influences on health outcomes.
Assess the implications of the social determinants of health for clinical and public health practice. practice.
RESOURCES
DETERMINANTS OF HEALTH: BEYOND MEDICINE
Health is
multi-factorial and has many determinants.
There are
modifiable and non-modifiable determinants of health. While non-modifiable
determinants of health such as biology and genetics cannot be changed,
determinants such as education, income, and the physical environment etc can be
changed.
Over the last
twenty years, a compelling body of evidence has documented the effect of social
factors on health(1). Social factors of health can also
be called social determinants of health. Some studies have attributed up to 60
percent of preventable mortality to socioeconomic
factors(2).
Arising from this understanding of the
complex ways in which health determinants at different levels impact health
outcomes, Prof. Michael Marmot, a proponent of the social determinants of
health model states that in treating patients, doctors need to address
'individual behavior in social perspective' (p.688)(1). As we will see a little later in this topic, Prof. Marmot and
others have since also provided persuasive evidence showing that lower socioeconomic status is
generally associated with a higher
likelihood of exposure to risk behaviors. Such evidence has served to
demonstrate the powerful interlinkages between the biological, social, and
psychological dimensions of health.
These developments have led to increasing calls to integrate knowledge about the social determinants of health in medical education and clinical

practice. There is also a growing body of guidance on how clinicians might address the social determinants of health in the practice of medicine.
In this module, we examine key concepts related to the social determinants of health. We then explore some interesting work of pioneering physicians who drew attention to the association between social disadvantage, deprivation, and ill-health. We will then finally round off this module by reflecting on how clinicians can address the social determinants of health in clinical practice.
REFERENCES
1. Marmot M. The health gap: Doctors and the social determinants of health.
Scand J Public Health. 2017;45(7):686-93.
2. Schroeder SA. We can do better — improving the health of the American
people. New England Journal of Medicine. 2007;357(12):1221-8.
EQUALITY & INEQUITY
Let’s continue to recap. What is health equality? How is it different from health equity?
Click on the arrow below to check if you got the answer right.
FROM DETERMINANTS TO THE WORLD HEALTH ORGANIZATION (WHO) SOCIAL DETERMINANTS OF HEALTH FRAMEWORK
So far, we have revised the idea that health has multiple determinants and that social conditions such as education, income and living environments play a major role in shaping who gets sick, when, and with what consequences. To work with these ideas in clinical and public health practice, we need a clear framework that shows how different types of determinants fit together and lead to patterned differences in health outcomes within and between populations.
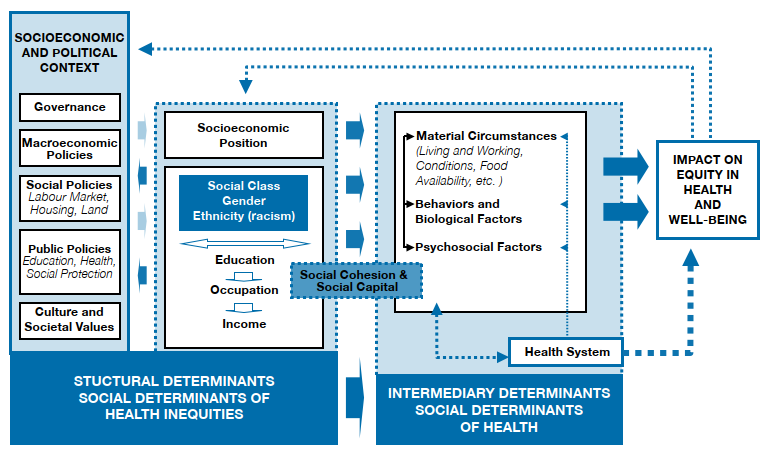
In the video by Dr. Ranil Appuhamy below, you will be introduced to the World Health Organization’s Social Determinants of Health framework. This framework distinguishes between structural determinants (for example, governance, macro economic and social policies, and cultural values that shape people’s socioeconomic position) and intermediary determinants (for example, material living conditions, psychosocial factors, health related behaviors and health care access). As you watch, focus on how structural determinants influence intermediary determinants, and how this interaction helps to explain why health is systematically better in some groups and worse in others.
The WHO Social Determinants of Health Framework
As you study the diagram, trace one example: for instance, how does education policy (a structural determinant) influence someone's occupation and income (socioeconomic position), which then affects their material circumstances and behavioral, biological, and psychological factors (intermediary determinants), and ultimately their health?
TRAVERSING THE BOUNDARIES OF MEDICINE: Sir Michael Marmot
Up to this point, you have seen how the WHO framework explains the pathways from structural and intermediary determinants to health outcomes. Learning Outcome 2 asks you to go a step further: How do these determinants produce systematic differences in health within and between populations?
In this first video, we will review Sir Michael Marmot's idea of the social gradient in health. His work on the Whitehall studies shows that, even within one country and one health care system, people in lower occupational and social positions have worse health and shorter life expectancy than those above them. As you watch, focus on how Marmot links everyday social conditions, such as control at work, income and status, to graded differences in health across the whole population, not just between the very rich and the very poor.
TRAVERSING THE BOUNDARIES OF MEDICINE: Rudolf Virchow & Thomas McKeown
As you watch the two short videos, focus on these questions:
• Which social and economic conditions do Virchow and McKeown highlight in their explanations of disease and mortality?
• How do those conditions help explain differences in health between social groups, or changes in health across time? Use their arguments to strengthen your explanation of how social determinants of health generate differences in health outcomes within and between populations.
HOW STRUCTURES AND BIAS DRIVE HEALTH INEQUITIES
In the previous section, we saw different physicians use a social model of health to explain
health and disease. They highlighted the significance of the social determinants of health in
generating health inequities or contributing to good health.
In this final section, through brief examples, you will review three ideas: structural violence, structure and agency, and implicit bias, that help to show how unfair social arrangements and hidden stereotypes can lead to worse health for some groups.
A MULTILEVEL LENS ON HEALTH IN PRACTICE
This video introduces McLeroy et al.’s Social Ecological Model (1988) as a multilevel lens you can apply to clinical and public health decision‑making, showing why health behaviours and outcomes rarely depend on individual choices alone. You will review how influences at five levels—from intrapersonal factors to families, organisations, communities and public policy—interact to shape patterns like tobacco use, and you will see how this framework gives you concrete prompts for action at each level when assessing patients and planning interventions.
TOGGLE TIME
 .
. 